-
Best Australian Pokies Best Payout
Play Free 777 Pokies Online
What Are the Best Australian Pokies to Win Big On
What Are the Best Online Pokies with Low Minimum Deposits for Real Money in Australia
New Australian Pokies Accepting PayID
What Are the Best Strategies to Win in Online Pokies with Bonus Rounds in Australia
Tips for Winning Top Australian Pokies
What Online Casinos Offer Free Play Pokies with Welcome Bonuses in Australia
Australian Slot Games
Payout Ratio Pokies with Welcome Bonus
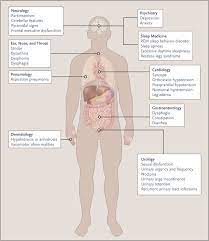
Multisystem issues are often a consequence of a failing body system and identification and consideration to determine the underlying cause of illness is essential.
Multisystem issues are often a consequence of a failing body system
Signature Assignment Title: Pathophysiology
Signature Assignment Description/Directions: Multisystem issues are often a consequence of a failing body system and identification and consideration to determine the underlying cause of illness is essential. Though illness may create multisystem issues and may affect many body systems, for this assignment you will focus on three: renal, pulmonary, and circulatory systems.
This PowerPoint® (Microsoft Office) or Impress® (Open Office) presentation should be a minimum of 20 slides, include a title and reference slide, and detailed speaker notes and a recorded audio clip on all content slides.
You will discuss a specific illness, disorder or disease and the interrelationship with the renal, pulmonary, and circulatory systems, specifically identifying and describing how an alternation in one systems may affect one or more of other two body systems.
Explain how the body tries to compensate for a disorder, with assistance or reliance on another body system. Your submission should include three graphics or illustrations and a minimum of 5 peer-reviewed sources to support any of your perspective.
Please review the module’s Signature Assignment Rubric before starting this assignment to ensure that you are meeting all the essential requirements. This presentation is worth 400 points for quality content and presentation.
Multiple Organ System Failure
Kindred Hospitals can create an expert care plan to assist you or your loved one on the path to recovery from multiple organ system failure – serving as your bridge from the ICU to home.
What Is Multiple Organ System Failure?
When the inflammation from a severe infection or injury causes dysfunction in two or more organ systems, this is called multiple organ system failure. Often, patients experiencing multiple organ system failure have already been admitted to the hospital to treat underlying or connected conditions, such as hypoperfusion and hypermetabolism. Unfortunately, multiple organ system failure, also known as Multiple Organ Failure (MOF) or Multiple Organ Dysfunction Syndrome (MODS), can be fatal. There’s no single answer to what causes organ failure, and depending on the patient, there can be many factors involved. However, organ failure can be triggered by sepsis, an extreme response to an infection which causes inflammatory chemicals to be released into the bloodstream.
Considering how series of a condition multiple organ system failure is, it is critical for medical staff to be aware of the signs of organ failure. Organ failure symptoms include low grade fever, tachycardia, and tachypnea in the first 24 hours. Within the following 24-72 hours, lung failure may set in. This can be followed by bacteremia, as well as renal, intestinal, and liver failure. Within two to three weeks, encephalopathy, cardiac failure, and death may occur.
Multiple Organ Failure Symptoms By Organ
Multiple organ dysfunction syndrome can affect any or all of six organ systems: respiratory, cardiovascular, renal, hepatic, neurologic and hematologic. Critically ill patients with signs of failure in any of these systems need immediate clinical intervention to recover.
Lung/Respiratory
Respiratory failure can happen as a result of injury, infection, or surgical complications. Signs include difficulty breathing, anxiety, sweating, and bluish skin. Patients with respiratory failure may become ventilator dependent during their care.
Heart/Cardiovascular
Heart failure can occur when the heart muscle is too weak or stiff to pump blood properly. Signs include irregular heartbeat, weakness, inability to exert oneself, and swelling in the lower extremities. Heart failure can lead to both kidney and liver damage, as the blood flowing from the heart to the kidneys may decrease, and the liver may experience pressure from fluid buildup.
Kidney/Renal
Acute renal failure happens when the kidneys are not able to filter waste from the blood. When the kidneys lose this ability, dangerous levels of waste can accumulate, and the blood’s chemistry may become unbalanced. Signs include nausea, seizures, reduced urine production, swelling in the lower extremities, and chest pain.
Liver/Hepatic
Liver failure occurs when large parts of the liver become damaged beyond repair and the liver can no longer function. It can happen gradually, over many years, or acutely, within as little as 48 hours. Signs include nausea, abdominal pain and swelling, and yellowing of the eyes and skin.
Brain/Neurologic
Because the brain controls the other systems of the body, neurological dysfunction can take many forms. However, an altered state of consciousness is a common manifestation of neurological failure associated with MODS.
Blood/Hematologic
Bleeding in the gastrointestinal tract or breaks in the skin is common when someone is experiencing multiple organ failure. This can be very difficult to control or stop.
What Is The Best Path To Multiple Organ Failure Recovery?
Currently, there is no drug or therapy that can reverse organ failure. However, organ function can recover to some degree. Doctors have discovered that some organs recover better than others. Multiple organ failure recovery can be a slow and challenging process. Early detection is very important when treating multiple organ failure. ICU treatment at a traditional hospital is typically only the first stage of recovery. Once a patient has moved into transitional care, there are options for supporting specific organ systems, including mechanical ventilation and dialysis.
“When creating a care plan for patients with multiple organ system failure, the team at Kindred is dedicated to helping each progress at their own pace,” says Dr. Sean Muldoon, Senior Vice President and Chief Medical Officer for Kindred Healthcare’s Hospital Division. “We build custom plans based on the organs that are impacted and the extent of the damage. Our goal is to help stop the organ failure process and reverse effects when possible.”
Success Spotlight: Kay’s Story
Kay had endured a long waiting period for a heart transplant as her birth heart was failing. When she was finally able to have the transplant performed at the beginning of the year, she unfortunately developed multi-organ failure and numerous complications, including acute respiratory failure. Her physicians worked hard to stabilize her condition and finally managed to wean her from the ventilator nearly a month after her transplant. Kay was able to be transferred to Kindred Hospital where she would begin to receive additional respiratory therapy to strengthen her lungs, and rehabilitation to enable her to reclaim her independence and return home.
Kay was completely dependent on her team of caregivers for all her needs as she was extremely debilitated and couldn’t even lift her arms or legs on her own. She was guided by her physical and occupational therapists who worked with her seven days a week until she was finally able to stand and walk on her own and take care of her daily needs. Her speech pathologist helped her reclaim the ability to speak using a voice valve at first and then, when the breathing tube had been removed, Kay was able to once again speak with her own voice and begin to drink and eat a normal diet.
“This was a long journey,” Kay shared before she was discharged. “I had to fight confusion and depression along the way, but I’m grateful for the care I received and for having the support of my husband and daughter every step of the way.”
Attachments
