-
Best Australian Pokies Best Payout
Play Free 777 Pokies Online
What Are the Best Australian Pokies to Win Big On
What Are the Best Online Pokies with Low Minimum Deposits for Real Money in Australia
New Australian Pokies Accepting PayID
What Are the Best Strategies to Win in Online Pokies with Bonus Rounds in Australia
Tips for Winning Top Australian Pokies
What Online Casinos Offer Free Play Pokies with Welcome Bonuses in Australia
Australian Slot Games
Payout Ratio Pokies with Welcome Bonus
Hysterectomy and Hypertension Study. Throughout this course you will be developing a formal, Evidence-Based Practice Project Proposal. The proposal is the plan for an Evidence-Based Practice Project designed to address a problem,..
Hysterectomy and Hypertension Study
Assessment Descriiption
Throughout this course you will be developing a formal, Evidence-Based Practice Project Proposal.
The proposal is the plan for an Evidence-Based Practice Project designed to address a problem, issue, or concern in the professional work setting.
Although several types of evidence can be used to support a proposed solution, a sufficient and compelling base of support from valid research studies is required as the major component of that evidence.
Proposals are submitted in a format suitable for obtaining formal approval in the work setting. Proposals will vary in length depending upon the problem or issue addressed, but they should be between 3,500 and 5,000 words.
The cover sheet, abstract, references page, and appendices are not included in the word count. Review the paper template (with abstract) provided in the Student Success Center and “Evidence-Based Practice Project Proposal Format,” located in the Class Resources, for guidance on preparing abstracts.
Section headings and letters for each section component are required. Responses are addressed in narrative form in relation to that section. Evaluation of the proposal in all sections is based upon the extent to which the depth of content reflects graduate-level critical thinking skills.
This project proposal contains six formal sections:
Section A: Problem Descriiption
Section B: Research Support
Section C: Proposed Solution
Section D: Change Model
Section E: Implementation Plan
Section F: Evaluation of Process
Each section (A-F, to be completed in Topics 1-6) was previously submitted as a separate assignment so your instructor could provide feedback for revision (refer to each previous topic for those specific assignments and instructor feedback).
The final paper will consist of the completed project (with revisions to all sections), title page, abstract (review the template with abstract, located in the Student Success Center), reference list, and appendices.
Appendices will include a conceptual model for the project, handouts, data and evaluation collection tools, a budget, a timeline, resource lists, and approval forms.
Objective: Hysterectomy is the second most common surgery performed mainly for benign uterine pathologies in females. The association between hysterectomy and the subsequent risk of hypertension remains controversial.
This study investigated the risk of developing hypertension in women who had a hysterectomy.
Design: Population-based retrospective cohort study.
Setting: We used the Taiwan National Health Insurance Research Database with claims data of 1 million randomly selected insured individuals.
Population: Women with and without hysterectomy and bilateral salpingo-oophorectomy, aged 30-49 years, were identified in 2000-2013 from the insurance data.
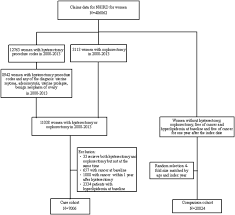
Methods: From the claims data, we identified 6674 women with hysterectomy without hypertension at the time of the surgery. The comparison cohort were 26 696 women randomly selected from women without hysterectomy and hypertension, matched by age and the year hysterectomy was performed.
Adjusted hazard ratio (aHR) of hypertension was estimated after controlling for comorbidities.
Main outcome measure: Prediction for hypertension following hysterectomy for benign disease.
Results: Both cohorts had a median age of 43.9 years. After a median follow up of 6.4 years, the incident hypertension was higher in the hysterectomy cohort than in the comparison cohort, with an adjusted hazard ratio (aHR) of 1.35 [95% confidence interval (CI) 1.27-1.44].
The incidence increased with age, with a higher aHR in hysterectomised women aged 40-49 years (aHR 1.37, 95% CI 1.06-1.83) than in those aged 30-39 years (aHR 1.22, 95% CI 1.02-1.46).
Conclusion: Findings in this study suggest that women with hysterectomy are more likely to be diagnosed with hypertension in the follow-up period.
Tweetable abstract: Women with hysterectomy before 50 years of age are at an increased risk of developing subsequent hypertension.
Plain language summary: Hysterectomy is one of the most common surgeries for women with benign uterine disease. Hysterectomy may lead to a sudden decline in the production of sex hormone (estrogen and progesterone), which is responsible for vessel wall endothelial dysfunction leading to hardening of arteries and subsequent hypertension. However, the association between hysterectomy and risk of hypertension remains controversial.
This study investigated whether premenopausal women have an elevated risk of hypertension after hysterectomy. This study employed the Taiwan National Health Insurance Research Database to identify 6674 women 30-49 years old who had a hysterectomy between 2000 and 2013, and a comparison group of 26 696 women who did not have a hysterectomy matched by age.
Women in both the groups had no hypertension at baseline (recruiting date or within 1 year after recruiting date). By the end of 2013, we found that 1196 (17.9%) and 3613 (13.5%) women had developed hypertension in the hysterectomy and the comparison groups, respectively. The hypertension incidence was 1.4-fold greater in the hysterectomy group than in the control group (27.8 versus 20.2/1000 person-years).
Attachments
