-
Best Australian Pokies Best Payout
Play Free 777 Pokies Online
What Are the Best Australian Pokies to Win Big On
What Are the Best Online Pokies with Low Minimum Deposits for Real Money in Australia
New Australian Pokies Accepting PayID
What Are the Best Strategies to Win in Online Pokies with Bonus Rounds in Australia
Tips for Winning Top Australian Pokies
What Online Casinos Offer Free Play Pokies with Welcome Bonuses in Australia
Australian Slot Games
Payout Ratio Pokies with Welcome Bonus
Demonstrate an awareness of and responsiveness to the larger context and system of health care, as well as the ability to call effectively on other resources in the system to provide optimal health care” (University of Maryland Medical Center, 2022).
Demonstrate an awareness of and responsiveness to the larger context
Assignment 5: Systems-based Practice in Nursing Systems-based practice in nursing involves patient care from a wider perspective and requires practitioners to “demonstrate an awareness of and responsiveness to the larger context and system of health care, as well as the ability to call effectively on other resources in the system to provide optimal health care” (University of Maryland Medical Center, 2022).
This approach includes special attention to cost awareness, risk benefit analysis, patient care quality advocacy, inter-professional teamwork, system error identification, and developing and implementing systems solutions.
Assignment Criteria: Develop a scholarly paper that addresses the following criteria:
1. Cost Awareness
2. Risk benefit analysis
3. Patient care quality advocacy
4. Inter-professional teamwork
5. System error identification
6. Developing and implementing systems solutions
7. Questions to consider: a. How can I improve the care for my patients? b. How can I improve the system of care? c. How would you identify and prioritize change?
8. The scholarly paper should a. 4 to 6 pages, excluding the title and reference page. b. Include an introductory paragraph, purpose statement, and a conclusion. c. Include level 1 and 2 headings to organize the paper. d. Write the paper in third person, not first person (meaning do not use ‘we’ or ‘I’) and in a scholarly manner.
To clarify: I, we, you, me, our is not used. In addition, describing yourself as the researcher or the author should not be used. e. Include a minimum of two (2) peer-reviewed scholarly journal references( peer-review) to support the paper (review in Ulrich Periodical Directory) and be less than five (5) years old.
This blog post, focused on Systems-Based Practice in Nursing, continues our series about measuring nurse competency.
Systems-based Practice in Nursing involves patient care from a wider perspective. According to the University of Maryland Medical Center, this approach requires practitioners to “demonstrate an awareness of and responsiveness to the larger context and system of health care, as well as the ability to call effectively on other resources in the system to provide optimal health care.”
This approach also includes special attention to cost awareness, risk benefit analysis, patient care quality advocacy, inter-professional teamwork, system error identification, and developing and implementing systems solutions.
Demonstrating Competence in Systems-Based Practice
For nurses, the goal of systems-based practice is really to enhance the quality and safety of patient care. According to the Massachusetts Action Coalition, “Nurses play a critical role in the microsystems and macrosystems of health care delivery and the nurse of the future will recognize the importance of individual and group actions on quality and safe patient care.
Nurses will need to understand and initiate cost containment, resource allocation, patient advocacy and interdisciplinary collaboration to ensure the delivery of quality patient care.
Successful implementation of a systems-based practice would include interdisciplinary patient rounds, mechanisms for respectful interdisciplinary approaches to patient care issues and team building activities.”
Ultimately the goal “for the nurse of the future is to enhance and improve the interdisciplinary system of patient care while understanding the legal, political, regulatory and economic factors that influence the delivery of health care.”
Systems-Based Practice Education for Nurses
A 2020 article from the Agency for Healthcare Research and Quality (AHRQ) offers that education for medical professionals is changing. It states, “Historically, the approach to medical and nursing education has focused on establishing an understanding of body systems and the technical processes associated with diagnosis and treatment, with training often incorporating extensive memorization and practice of procedures until knowledge and basic proficiency is acquired.
Over the past two decades, the competency-based evolution in education has shifted the focus to outcomes or healthcare professionals’ competencies in patient safety education and systems-based practice.”
Assessing Competency in Systems-Based Practice
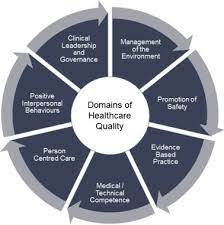
Evaluating systems-based practice competency is one of the most challenging areas of nurse competency management. Systems-based practice is an approach that applies to all areas of care, and it can be specialized by nursing role and practice environment. As an overall guide to how these evaluations work, envision a wider view of the components of the healthcare system and how an individual patient may interact with them.
A clinician who has mastered this competency will have knowledge of every direction care can lead and what is optimal for specific patients. Systems-based practice is one way to improve outcomes while paying special attention to health equity and improving healthcare delivery.
Some examples of systems-based practice in healthcare are approaching identified problems with the goal of fixing them rather than just relying on a workaround, working in interprofessional teams to enhance patient outcomes, and understanding how all the different care settings work together for patients.
Understanding the healthcare system and an individual professional’s role in it encourages clinicians to want to change the system for the better, leading to gains in safety and better health care for the larger population.
Our blog series about measuring nurse competency was developed to bring attention to all the attributes that contribute to truly competent nursing. In addition to this post, others address:
- Patient care
- Medical clinical knowledge
- Practice-based learning and improvement
- Professionalism
- Interpersonal Communication
Attachments
