-
Best Australian Pokies Best Payout
Play Free 777 Pokies Online
What Are the Best Australian Pokies to Win Big On
What Are the Best Online Pokies with Low Minimum Deposits for Real Money in Australia
New Australian Pokies Accepting PayID
What Are the Best Strategies to Win in Online Pokies with Bonus Rounds in Australia
Tips for Winning Top Australian Pokies
What Online Casinos Offer Free Play Pokies with Welcome Bonuses in Australia
Australian Slot Games
Payout Ratio Pokies with Welcome Bonus
Conflict with receiving the Influenza and COVID vaccination. Please use the Christian bible and scripture if so for examples and please cite the bible and any other references using APA Writing format.
Conflict with receiving the Influenza and COVID vaccination
Religious Exemption for Covid-19 and Influenza Vaccine , make it clear what my Christian religious belief, practice, or observance is. Please clarify the belief that is in conflict with receiving the Influenza and COVID vaccination. Please use the Christian bible and scripture if so for examples and please cite the bible and any other references using APA Writing format.
Impact of the influenza vaccine on COVID-19 infection rates and severity
Background
With a unique influenza season occurring in the midst of a pandemic, there is interest in assessing the role of the influenza vaccine in COVID-19 susceptibility and severity.
Methods
In this retrospective cohort study, patients receiving a laboratory test for COVID-19 were identified. The primary outcome was comparison of positive COVID-19 testing in those who received the influenza vaccine versus those who did not. Secondary end points in patients testing positive for COVID-19 included mortality, need for hospitalization, length of stay, need for intensive care, and mechanical ventilation.
Results
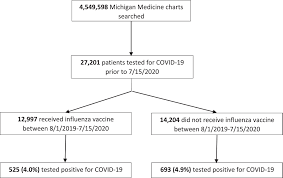
A total of 27,201 patients received laboratory testing for COVID-19. The odds of testing positive for COVID-19 was reduced in patients who received an influenza vaccine compared to those who did not (odds ratio 0.76, 95% CI 0.68-0.86; P < .001). Vaccinated patients testing positive for COVID-19 were less likely to require hospitalization (odds ratio, 0.58, 95% CI 0.46-0.73; P < .001), or mechanical ventilation (odds ratio, 0.45, 95% CI 0.27-0.78; P = .004) and had a shorter hospital length of stay (risk ratio, 0.76, 95% CI 0.65-0.89; P < .001).
Conclusion
Influenza vaccination is associated with decreased positive COVID-19 testing and improved clinical outcomes and should be promoted to reduce the burden of COVID-19.
Introduction
The novel coronavirus of 2019 (COVID-19) was first identified in Wuhan, China in December 2019, and was declared a public health emergency of international concern within one month. As of February 2021, more than 106 million confirmed cases of COVID-19 and over 2.3 million deaths have been reported globally.1 The clinical spectrum of illness caused by COVID-19 is broad, with severity of disease ranging from mild symptoms to acute respiratory distress syndrome with rapid deterioration.
Pre-existing cerebrovascular, liver, kidney and gastrointestinal diseases, as well as hypertension, diabetes, COPD, and age greater than 60 confer higher susceptibility to infection by COVID-19 and greater risk of mortality with infection.3,4 Importantly, patients with pre-existing cardiovascular risk factors are more likely to experience severe disease resulting from both direct and indirect cardiovascular complications of COVID-19, including myocarditis, arrhythmias, and venous thromboembolism.5
Clinical trials of dexamethasone6,7 and Remdesivir8 have shown a reduction in complications in very ill COVID-19 patients, and while effective vaccines against COVID-19 from both Pfizer-BioNTech and Moderna have been approved for use in the United States, they are not yet broadly available, making it imperative to explore the effects of currently available medical interventions that may lessen the susceptibility to and burden of disease.
With the influenza season upon us, there is interest in exploring the relationship between influenza vaccination and COVID-19 susceptibility and disease severity.
Recent studies have suggested that prior vaccination to pathogens such as tuberculosis and influenza may confer some protection against COVID-19.
An analysis of over 92,000 COVID-19 patients in a nonpeer reviewed study from Brazil found a 17% reduced odds of mortality, 8% lower odds of need for intensive care treatment and 18% lower odds of invasive respiratory support in those who received an influenza vaccine.
Separate epidemiologic studies in Italy and the United States found a correlation between increased vaccination rates in those aged greater than 65 years and decreased rates of COVID-19 deaths across different regions.
Using data from patients tested for COVID-19 within the Michigan Medicine healthcare system, we explored the relationship between influenza vaccination and positive COVID-19 testing. For COVID-19 positive patients, we compared disease severity and mortality risk between those who were vaccinated and unvaccinated against influenza.
Attachments
