-
Best Australian Pokies Best Payout
Play Free 777 Pokies Online
What Are the Best Australian Pokies to Win Big On
What Are the Best Online Pokies with Low Minimum Deposits for Real Money in Australia
New Australian Pokies Accepting PayID
What Are the Best Strategies to Win in Online Pokies with Bonus Rounds in Australia
Tips for Winning Top Australian Pokies
What Online Casinos Offer Free Play Pokies with Welcome Bonuses in Australia
Australian Slot Games
Payout Ratio Pokies with Welcome Bonus
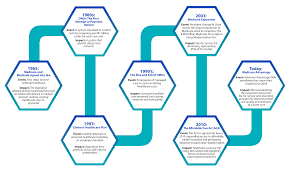
There is discussion regarding the evolution of healthcare payment models including value-based care. The Centers for Medicare and Medicaid Services (CMS) established value-based purchasing programs to encourage hospitals to report, and improve, outcome measures.
Evolution of healthcare payment models
There is discussion regarding the evolution of healthcare payment models including value-based care. The Centers for Medicare and Medicaid Services (CMS) established value-based purchasing programs to encourage hospitals to report, and improve, outcome measures. The goals also include improved quality and transparency of care delivered.
Locate the CMS value-based care website and review the various value-based programs. Example programs include End-Stage Renal Disease Quality Incentive Program (ESRD QIP), Hospital Value-Based Purchasing (VBP) Program, Hospital Readmission Reduction Program (HRRP), Hospital Acquired Conditions (HAC) Reduction Program, and the Skilled Nursing Facility Value-Based Program (SNFVBP).
Choose one program and write a short paper that considers the following questions:
1. Describe the program. What is the program intended to improve?
2. How does the program calculate performance payments or penalties?
3. How are hospitals or skilled nursing facilities performing today?
4. How has CMS modified the program in the past or recommends modifications in the future?
This written assignment should be completed as a single Word document and contain between 1,000 and 1,500 words. The paper should be double-spaced and formatted using the APA 7th edition manual.
Please ensure your outsource sources are cited and referenced according to APA formatting. Please create a title page which includes your name, date, course number, and assignment title. Papers will be graded based upon thoroughness, accuracy of information, and properly written communication, including grammar, mechanics, and organization.
The Evolution of Healthcare Payment Models: From Fee-for-Service to Value-Based Care
The healthcare payment landscape is changing rapidly. In the past, healthcare providers were typically paid on a fee-for-service basis. However, with the rise of value-based care models, this is starting to change. In this blog post, we will discuss the evolution of healthcare payment models and what it means for the future of healthcare.
The fee-for-service model is the traditional way that healthcare providers have been paid. Under this model, providers are reimbursed for each service that they provide. This type of payment incentivizes providers to see as many patients as possible and to order tests and procedures, even if they may not be necessary. As a result, this can lead to unnecessary care and higher healthcare costs.
The value-based care model is a newer way of paying for healthcare services. Under this model, providers are reimbursed based on the quality of care that they provide, not the quantity. This means that providers are incentivized to deliver high-quality care that leads to positive health outcomes for patients. In addition, value-based care models often include provisions for cost containment, which can help to keep healthcare costs down.
The shift from fee-for-service to value-based care is a major change in the healthcare landscape. This shift is being driven by a number of factors, including the Affordable Care Act, the rise of consumerism in healthcare, and the increasing focus on population health.
As a result of this shift, we are likely to see more value-based care models emerge in the coming years.
These models have the potential to improve the quality of care while also reducing healthcare costs. only time will tell if they will be successful in achieving these goals.
Health care is currently in the middle of a transition from a system of payment based on the volume of services provided (fee-for-service) to payment based on the value of those services (value-based care and alternative payment models).
The Center for Medicare & Medicaid Services has set a goal of increasingly tying Medicare payment to value. For example, CMS estimated that, as of January 1, 2016, nearly a third of Medicare payments were attributed to alternative payment models. Thus, for now, hospitals and health systems must exist in both the fee-for-service and value-based worlds. Specifically, they need to continue to serve and operate under the traditional, siloed payment systems, such as Medicare’s inpatient and outpatient prospective payment systems.
However, they also must begin to determine how they will take financial accountability for the quality and costs of an entire episode of care or attributed population, such as under the Comprehensive Care for Joint Replacement bundled payment or Accountable Care Organization programs.
Attachments
